G6PD Medication Safety Checker
Medication Safety Checker
Results
When you have G6PD deficiency, certain medications can trigger a dangerous drop in red blood cells - a condition called hemolytic anemia. This isn't just a theoretical risk. In 2021, a 28-year-old man in the U.S. received rasburicase for tumor lysis syndrome without being tested for G6PD deficiency. His hemoglobin plummeted from 13.4 g/dL to 3.1 g/dL in under 72 hours. He needed 10 units of blood. This kind of emergency is preventable. The key? Knowing which drugs to avoid - and making sure your doctors know too.
What Is G6PD Deficiency?
G6PD deficiency is a genetic condition that affects how your red blood cells handle stress. Your body makes an enzyme called glucose-6-phosphate dehydrogenase (G6PD) to protect those cells from damage caused by oxidation. If you’re deficient, that protection is weak. When you take certain drugs, eat fava beans, or get a serious infection, your red blood cells can break apart rapidly. This isn’t a slow, chronic problem like sickle cell disease. It’s sudden. And it can be life-threatening.
It’s not rare. Around 400 million people worldwide have it. In some regions, it’s common because it offers partial protection against malaria. That’s why it’s most widespread in Africa, the Mediterranean, and Southeast Asia. But it’s found everywhere. In the U.S., about 1 in 10 African American males carries the deficiency. And here’s something many don’t know: 15% of women with the gene can also have hemolytic episodes. That’s because of how the X chromosome works - it’s not just a male condition.
Which Medications Are Dangerous?
The World Health Organization lists 87 medications that can trigger hemolysis in people with G6PD deficiency. Not all are equally risky. Some are absolute no-gos. Others are risky only at high doses. Here’s what you need to know:
- Rasburicase - Used to treat tumor lysis syndrome. It causes 100% hemolysis in deficient patients. The FDA issued a black box warning in 2023. Never give this without testing first.
- Methylene blue - Used for methemoglobinemia. In G6PD-deficient patients, it causes severe hemolysis in 95% of cases. A 2023 Reddit post from a nurse described giving it to an undiagnosed patient - hemoglobin dropped from 14.2 to 5.8 in 48 hours. Three units of blood were needed.
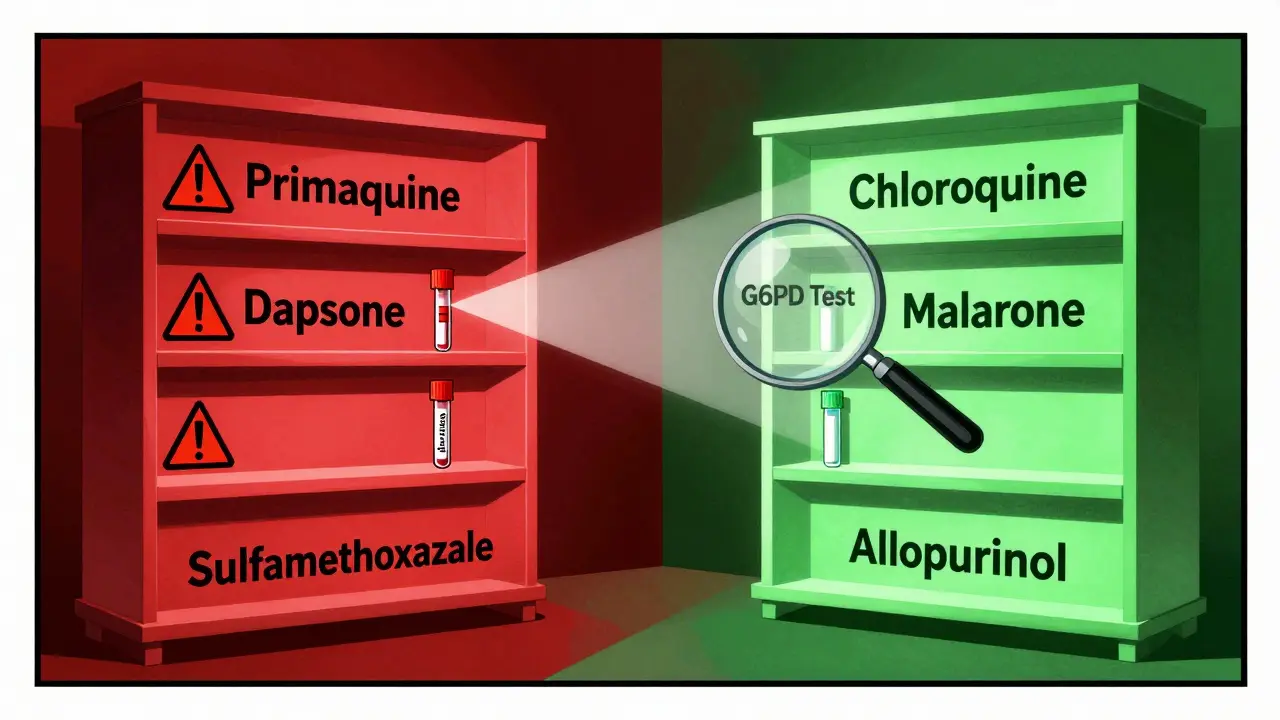
- Primaquine - A malaria drug. It kills the parasite, but also kills red blood cells in G6PD-deficient people. WHO guidelines say it’s unsafe for Class I and II patients. Even in Class III, it requires careful dosing and monitoring.
- Dapsone - Used for leprosy and some skin conditions. At doses above 50 mg daily, it causes hemolysis in 80% of deficient patients. Many doctors still prescribe it without checking G6PD status.
- Sulfonamides - Antibiotics like sulfamethoxazole. Risk is real, though not as high as the others. Still, avoid them unless no alternatives exist.
Some drugs get flagged based on very little evidence. For example, glyburide (a diabetes pill) has a warning on 92% of its labels worldwide - but only 17 cases of hemolysis have ever been documented since 1965. That’s why experts say: Don’t rely on labels alone. Ask for testing.
Safe Alternatives Exist
You don’t have to go without treatment. There are safe options for almost every situation:
- For malaria prevention: Chloroquine is safe in all G6PD deficiency classes. Atovaquone-proguanil (Malarone) is the top choice for travelers. WHO data shows 95% of deficient travelers using Malarone avoided hemolysis.
- For malaria cure: Artemisinin-based combination therapies (ACTs) are safe and effective. Tafenoquine is now approved - but only if you’ve been tested and cleared. The FDA requires G6PD testing before prescribing it.
- For methemoglobinemia: Instead of methylene blue, use ascorbic acid (vitamin C). It’s slower, but safe.
- For tumor lysis: Allopurinol replaces rasburicase. It doesn’t work as fast, but it doesn’t destroy red cells.
In Thailand, a hospital implemented a rule: no primaquine without a G6PD test. Over four years, hemolytic crises dropped from 15.2% to 0.3% among 4,327 patients. That’s not luck. That’s policy.
Testing Is the Foundation
You can’t manage what you don’t know. The problem? Many doctors still don’t test. A 2022 survey of 1,247 G6PD-deficient people found that 68% had at least one hemolytic episode - and 42% said their providers didn’t know the risks.
The best test? The fluorescent spot test. It’s fast - results in 15 minutes. It’s accurate - 98.7% sensitivity, 99.2% specificity. The WHO recommends it for newborns in high-prevalence areas. In Saudi Arabia, universal newborn screening cut hospital admissions for hemolytic crises by 78% between 2010 and 2020.
But here’s a critical detail: Don’t test right after a hemolytic episode. Your enzyme levels rebound over time. If you test too soon, you might get a false negative. Wait at least 3 months after an episode for accurate results.
Now, there’s even better news. In January 2024, the FDA approved the first point-of-care G6PD test that gives results in 8 minutes. It’s 99.1% accurate. This is huge for ERs, clinics, and travel clinics. No more waiting days for lab results.
What About Other Triggers?
Medications aren’t the only danger. Fava beans can trigger hemolysis - especially in Mediterranean populations. Infections like pneumonia or hepatitis can too. Even some herbal supplements, like neem or tea tree oil, carry risk. Avoid them unless you know they’re safe.
And yes - stress matters. Severe emotional stress, intense exercise, or extreme heat can increase oxidative load. If you’re G6PD deficient, listen to your body. Don’t push through fatigue or illness.

Why Isn’t Everyone Tested?
It’s not about cost. The test costs less than $5 in most countries. It’s about awareness.
In the U.S., only 12 states require newborn screening. In Africa, only 18 of 47 WHO countries have national programs. The Global Fund has invested $127 million to fix this - but progress is slow.
And here’s the irony: G6PD deficiency is one of the most common inherited conditions in the world. Yet, it’s rarely on a doctor’s radar unless they’ve seen a case. That’s why patient advocacy matters. If you’re diagnosed, carry a card. Tell your pharmacist. Ask your doctor: “Have you tested me for G6PD?”
What’s Next?
Science is catching up. Researchers are testing N-acetylcysteine (NAC) to protect red cells during treatment with risky drugs like primaquine. Early lab results show a 75% reduction in hemolysis. Phase I trials for a recombinant G6PD enzyme replacement therapy begin in late 2024. That could change everything.
For now, prevention is everything. If you or someone you know has G6PD deficiency, the goal is simple: avoid triggers, know your safe alternatives, and get tested before any new medication.
One patient in Perth, Australia, told her pharmacist about her diagnosis after a hospital stay. The next time she got a prescription for sulfamethoxazole, the pharmacist flagged it, called her doctor, and got her switched to a safer antibiotic. No crisis. No hospital. Just good communication.
That’s the standard we should all expect.
Can G6PD deficiency be cured?
No, G6PD deficiency is a genetic condition and cannot be cured. But it can be managed effectively. With proper avoidance of oxidative triggers and safe medication choices, most people live normal, healthy lives without any hemolytic episodes.
Is G6PD deficiency only a problem for men?
No. While the gene is on the X chromosome and affects males more often, women can also be affected. About 15% of female carriers have low enough enzyme levels to experience hemolysis, due to random X-chromosome inactivation. This is often overlooked, leading to misdiagnosis or delayed care.
Can I get tested if I’ve never had symptoms?
Yes. Many people with G6PD deficiency never have symptoms unless exposed to a trigger like a drug or infection. If you’re from a high-prevalence region (Africa, Mediterranean, Southeast Asia), or have a family history, testing is recommended even without symptoms. It’s especially important before surgery, anesthesia, or starting new medications.
Are all malaria drugs unsafe for G6PD deficiency?
No. Artemisinin-based combination therapies (ACTs) are completely safe. Chloroquine is also safe. Tafenoquine is safe only after testing confirms sufficient enzyme activity. Primaquine is dangerous for Class I and II patients. Always confirm the specific drug and your G6PD class before use.
What should I do if I accidentally take a risky medication?
Seek medical help immediately. Symptoms of hemolysis include dark urine, jaundice (yellowing of skin/eyes), extreme fatigue, shortness of breath, and rapid heartbeat. Blood tests can confirm a drop in hemoglobin. Treatment involves stopping the drug, hydration, and sometimes blood transfusions. Early intervention prevents kidney damage and other complications.





9 Comments
Mariah Carle- 4 March 2026
I just want to say... 🤔 G6PD deficiency isn't just a medical condition-it's a silent epidemic. We treat it like a footnote when it should be front and center. Why do we wait for someone to nearly die before we ask, 'Did you get tested?' 🥲
Justin Rodriguez- 6 March 2026
I work in a rural ER and see this way too often. Last month, a 32-year-old woman came in with dark urine after taking sulfa for a UTI. She’d never been tested. Her Hb was 4.9. We gave her fluids, held the meds, and called hematology. She’s fine now. But she didn’t know she was at risk. We need standardized screening before prescribing anything risky. It’s not complicated. It’s just not prioritized.
Megan Nayak- 8 March 2026
Let’s be real-this whole thing is a scam engineered by Big Pharma to sell more tests. 🤨 The WHO lists 87 drugs? That’s not science, that’s fearmongering. I’ve read the actual studies-most of those drugs have ZERO proven cases of hemolysis in real-world settings. And don’t get me started on ‘methylene blue causes 95% hemolysis’-that’s from one nurse’s Reddit post. Where’s the double-blind data? Where’s the control group? 🤷♀️
Sharon Lammas- 8 March 2026
There’s something deeply human here that gets lost in the clinical data. G6PD deficiency isn’t a defect-it’s an evolutionary adaptation. It’s why so many people from malaria zones carry it. We call it a 'deficiency,' but really, it’s a shield. And now we’re punishing people for having a natural defense. Maybe we need to reframe this-not as a medical liability, but as a biological legacy. We owe it to those populations to honor that, not just fear it.
marjorie arsenault- 9 March 2026
If you’re reading this and you’ve never been tested-do it. Seriously. It’s a quick finger prick. Costs less than your coffee. You could save your life-or your child’s life. And if you’ve been diagnosed, tell your pharmacist. Tell your mom. Tell your dentist. You’re not being dramatic. You’re being smart. 💪 And if you’re a provider? Test before you prescribe. It’s not optional anymore.
Deborah Dennis-10 March 2026
I’m so tired of this. 'Safe alternatives exist'? No. They don’t. Allopurinol? Slower? That’s code for 'less effective.' And 'Malarone is safe'? Who’s paying for that? $150 a dose. Meanwhile, chloroquine is $2. But we don’t use it because it’s 'outdated.' This isn’t medicine. It’s privilege. And the people who get hurt? They’re the ones who can’t afford to be 'careful.'
Diane Croft-11 March 2026
I’m from Nigeria, and I’ve seen what happens when you don’t test. My cousin died at 19 after being given primaquine for malaria. He never knew he had it. Now, I run a small nonprofit that does free G6PD testing at community clinics. We’ve tested over 3,000 people. We’ve prevented 17 hemolytic crises. It’s not glamorous. But it’s life-saving. You don’t need a lab. You just need to care.
Donna Zurick-11 March 2026
Just had my first G6PD test last year. Never had symptoms. Never even thought about it. Now I carry a card in my wallet. My pharmacist knows. My doctor knows. My mom knows. It’s not a big deal. It’s just one more thing to know about your body. And honestly? It’s kind of empowering. Like you’re in on a secret that could save you.
Tobias Mösl-12 March 2026
You think this is about health? Think again. This is about control. The FDA approves a new $200 test? The WHO pushes screening? Big Pharma is pushing the narrative so they can sell you lifelong 'safe' meds that cost 10x more. They want you scared. They want you dependent. And they want you paying. Wake up. The 'black box warning' on rasburicase? That’s not safety-it’s liability insurance. And you’re falling for it.